
The Silent Drop: Detecting Orthostatic Hypotension in Parkinson’s...
We are excited to see so many of you join our FMEP courses. Several of...
0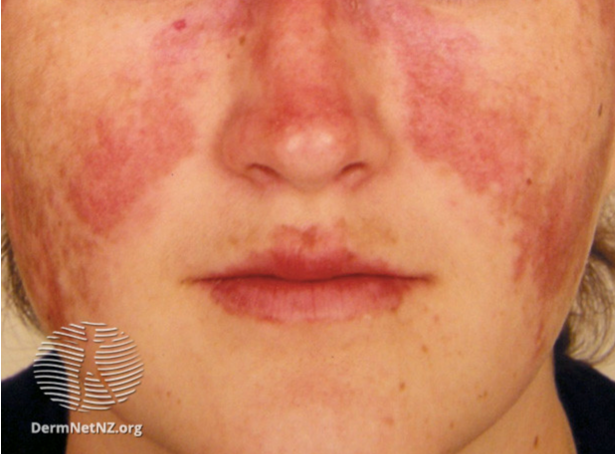
Just a reminder… pay attention to the questions. Here are our general tips one more time:
1. Pay attention to the questions. Look carefully at how many items you are being asked to list. If the question asks for five items, you will not get more marks if you list eight items; the examiner will look at the first five and allocate marks only for the first five answers – so be careful. On a SAMP, if it is not clearly stated how many items you should list, look at the amount of points/marks being allocated for the question to get an idea of how many answers the examiner may be anticipating you write down.
2. Do not write lengthy answers. Most questions can be answered in 10 words or less!
3. Be specific when writing down investigations (hemoglobin instead of CBC; CT abdomen instead of CT).
4. Remember that trade names and generic names are both acceptable when writing down medications.
5. For more helpful tips, you can refer to CCFP’s SAMP instructions by clicking here.
SAMP
Rosalea Markus, a 37 year old female, comes in to see you with a 3-week history of profound fatigue. She used to run 40km but now can barely get through 10km. She also has had significant body aches and a new rash that has developed across her cheeks. She is a project manager for a large investment bank and her fatigue is significantly impacting her work. She is a lifelong non-smoker and drinks 3-4 drinks during the week. She takes an oral contraceptive and vitamin D. She has no known allergies. (9 points)
1. List your differential diagnosis for her rash. (2 points)
2. On history or physical exam, how could you differentiate the malar rash associated with SLE from some of the “mimickers� (1 point)
3. List three autoimmune markers you would order to help diagnose SLE. (3Â points)
4. What medication should most patients be started on with SLE? (1 point)
5. What is one risk factor associated with the medication listed in question 4 that all patients should be warned about and what screening would you recommend for them? (2 points)
Image by DermNet NZ, https://dermnetnz.org/
Creative Commons Attribution, https://creativecommons.org/licenses/by-nc-nd/3.0/nz/legalcode