
The Silent Drop: Detecting Orthostatic Hypotension in Parkinson’s...
We are excited to see so many of you join our FMEP courses. Several of...
0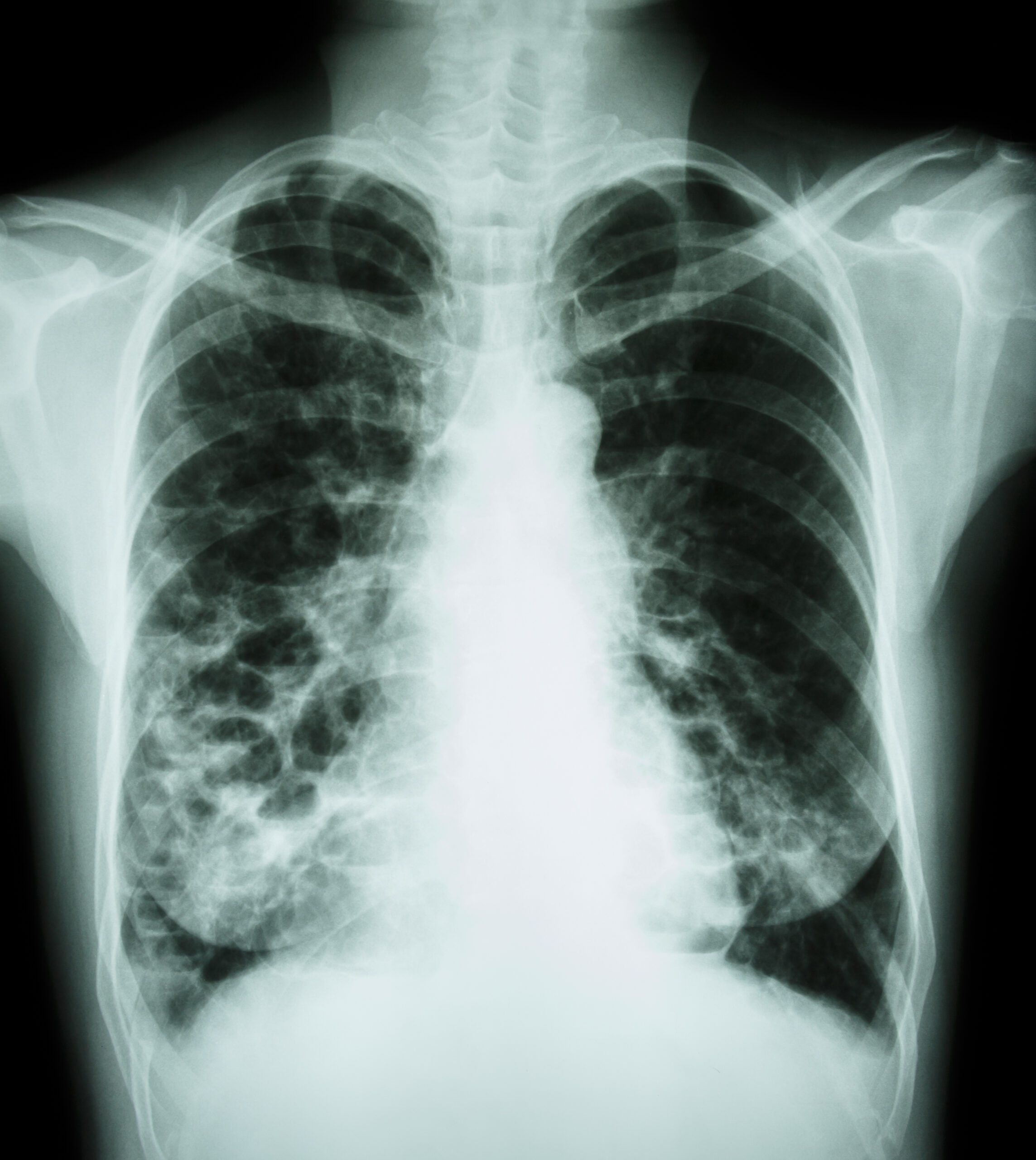
We are excited to see so many of you join our fall FMEP courses. Several of you have requested we continue to post more practice SAMPs, so here you go!
Just a reminder… pay attention to the questions. Here are our general tips one more time:
1. Pay attention to the questions. Look carefully at how many items you are being asked to list. If the question asks for five items, you will not get more marks if you list eight items; the examiner will look at the first five and allocate marks only for the first five answers – so be careful. On a SAMP, if it is not clearly stated how many items you should list, look at the amount of points/marks being allocated for the question to get an idea of how many answers the examiner may be anticipating you write down.
2. Do not write lengthy answers. Most questions can be answered in 10 words or less!
3. Be specific when writing down investigations (hemoglobin instead of CBC; CT abdomen instead of CT).
4. Remember that trade names and generic names are both acceptable when writing down medications.
5. For more helpful tips, you can refer to CCFP’s SAMP instructions by clicking here.
SAMP
Clarence Caugh is a 76 year old male. He has come to your office with a cough and intermittent shortness of breath for 14 months. He does not have fevers, chest pain, palpitations, leg swelling, or weight loss. His past medical history is significant for gout. He is taking Allopurinol. He is a non-smoker. He drinks 1-2 beers a month. He has not come to you earlier for these symptoms as he thought they were related to cold symptoms and would resolve on their own. On examination, he appears well. His BP is 132/78, HR is 86. Saturation is 99% on room air. His lungs sound clear. (8 points)
1. What are two characteristic findings on a CT scan for bronchiectasis? (2 points)
2. What two tests would you order to assess Clarence’s function if he is diagnosed with bronchiectasis? (2 points)
3. What are two non-pharmacologic management options for patients with bronchiectasis? (2 points)
4. True or false: Long-term antibiotic treatment with macrolides should be considered with patients who have ≥ 3 exacerbations a year. (1 point)
5. True or false: Acute exacerbations should be managed with a 14-day course of oral antibiotics. (1 point)
Helpful AJGP Resource:
https://www1.racgp.org.au/ajgp/2022/december/bronchiectasis